Dermato - Cosmetic Products
Unique, natural, multi-active and highly effective dermato-cosmetic products
| Products | Effect | Status | Partnering |
|---|---|---|---|
| Epi AA-C serum |
anti-inflammatory, anti-bacterial, anti-tumor and anti-viral effect inhibition of melanogenesis photoprotection (radical scavenger) skin regeneration |
Epi AA-C developed to market notified in EU & CH registration in China ongoing |
out-licensed for China available for other countries |
| Epi AA-T cream |
anti-inflammatory, anti-bacterial, anti-tumor and anti-viral effect wound healing photoprotection (radical scavenger) skin regeneration |
Epi AA-T development completed tolerability and stability test ongoing |
available for out-licensing |
| Epi AA-S cream |
high natural photoprotection and anti- inflammatory activity skin regeneration and hydration |
prototype developed finalization dependent on the country regulations in respect to SPF filters |
available for out-licensing |
EpiPharm AG: Pipeline 4/2023
Epi AA-C: The Lead Product
Epi AA-C multi-acting serum with outstanding efficacy designed to address
different skin problems
Multi-acting & multi-benificial
designed to address different skin disorders
- remarkable reduction of akne marks and hyperpigmentations
- effectively restores blemished skin and stimulates skin regeneration
- shows strong anti-pollution, anti-inflammatory and anti-bacterial effect
- acts against «skin growth disorders» (e.g. actinic keratosis)
- significantly increases skin density and elasticity (antiaging erffect)
Before Treatment
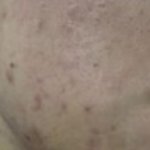
After Treatment
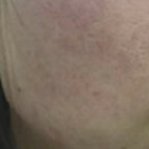
Outstanding efficacy
- demonstrated by clinical studies
- confirmed by product users (case series)
- developed and produced in Switzerland
- 100% natural & vegan
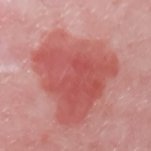
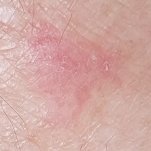

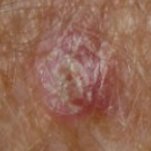
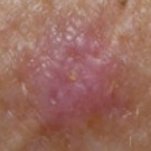
Seborrheic Keratois (SK) - Projects
First SK therapy that treats tumor formation and growth
SK treated with Epi-SK17
Dermoscopic image - Lesion clearance after treatment
EPI-SK 14, a phase I/II study with Artemether has successfully been completed. The data demonstrate a clinically relevant and statistically significant regression of SK lesions in size, color and texture. Regression continued markedly after treatment stop. The study results have been published online in the British Journal of Dermatology.
EPI-SK17 has been selected as lead product candidate based on properties which distinguish it from other artemisinin derivatives tested, including greater potency, and shorter duration of treatment. The product is about to enter phase IIb clinical development.
Before Treatment
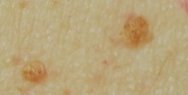
After Treatment

EPI-N06 - Project
Effective and lasting treatment of hyperpigmented spots
Age spot treatead with Epi-N06
Dermoscopic image – Significant regression in size and color
EPI-N06
is a topical, novel and effective treatment of melanocytic pigmented lesions which targets the melanin formation by synergistic mechanisms of action and by different pathways.
A phase I/II study has successfully been completed in melanocytic pigmented lesions (nevi and age spots) without tolerability issues. Data demonstrated clinically relevant regression of lesions size and color and a marked reduction of melanin in the epidermis.
Before Treatment
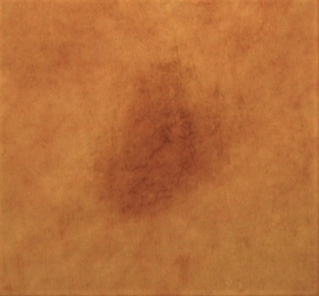
After Treatment

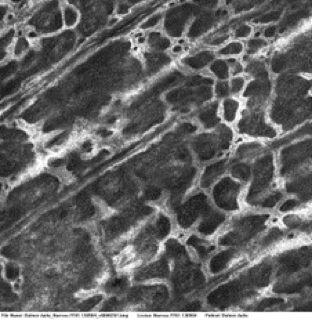
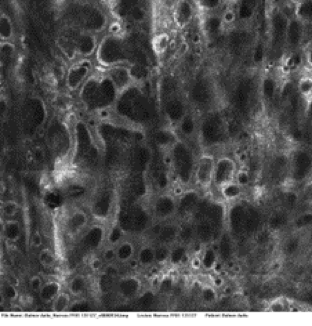
Confocal microscopy image – Relevant decrease of fluorescent melanin

